
University of North Texas Health Science Center at Fort Worth

HSC is one of the nation’s premier academic medical centers. Our six schools specialize in patient-centered education, research and health care.
Explore HSC

Colleges and schools
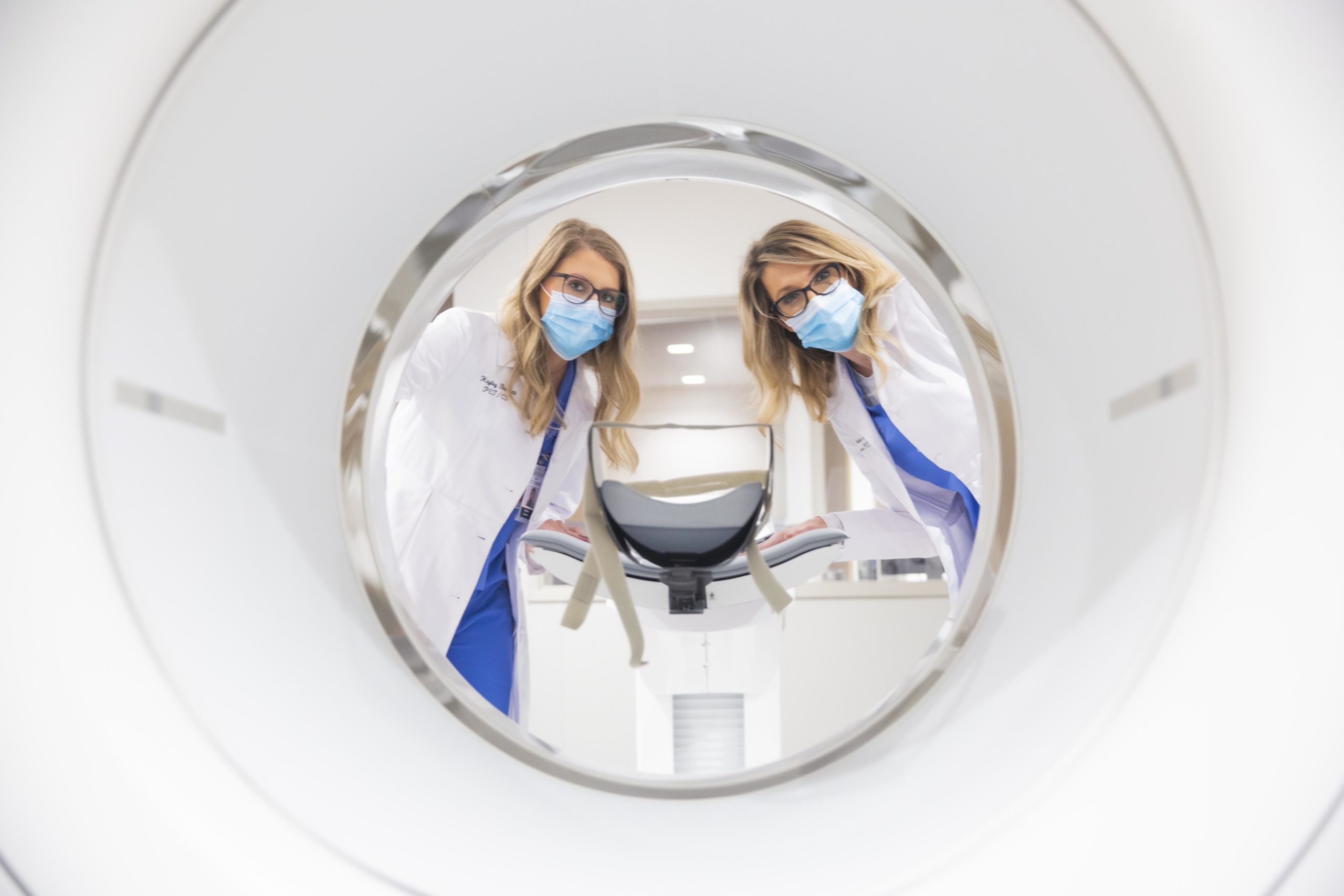
Research and innovation
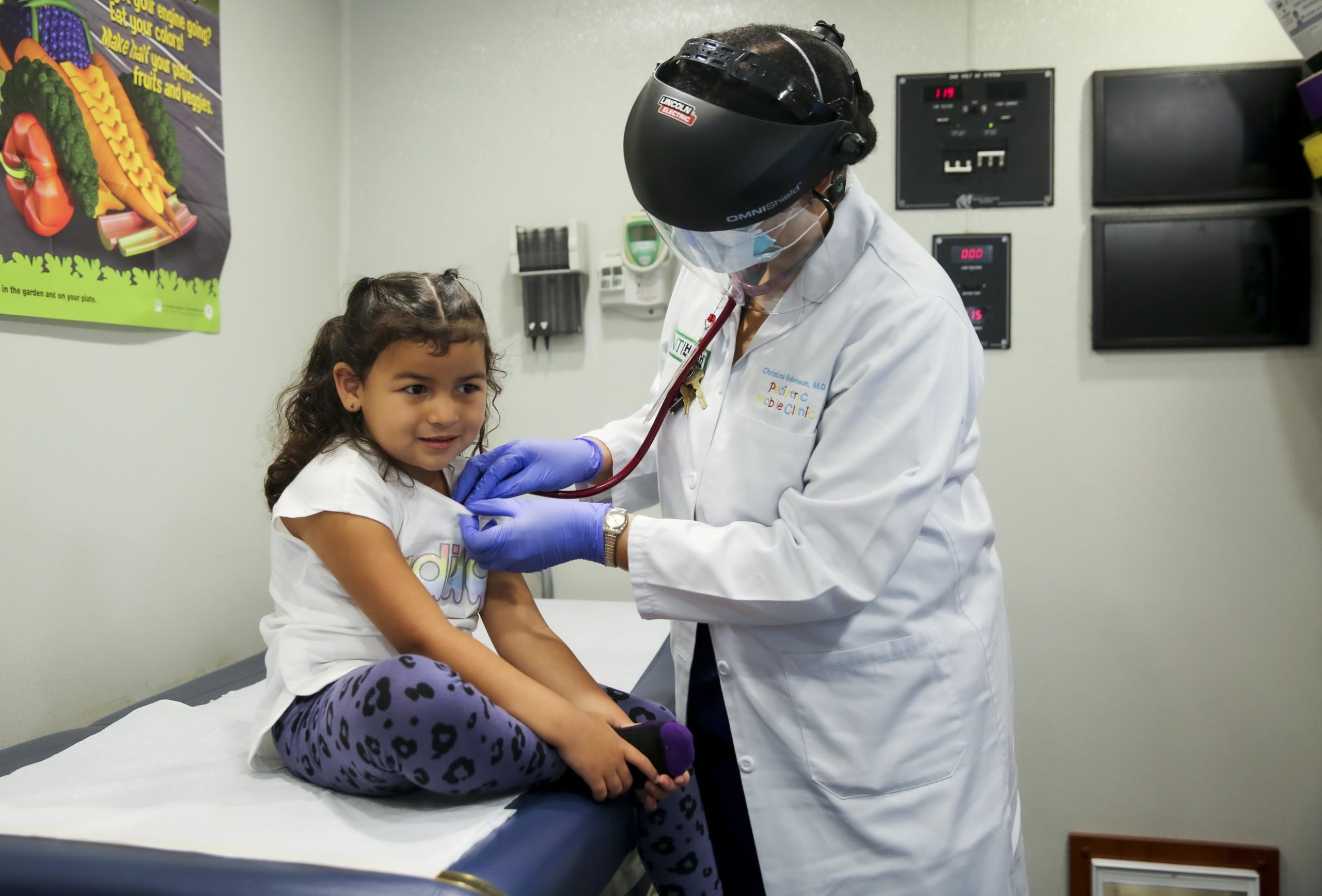
Patient care
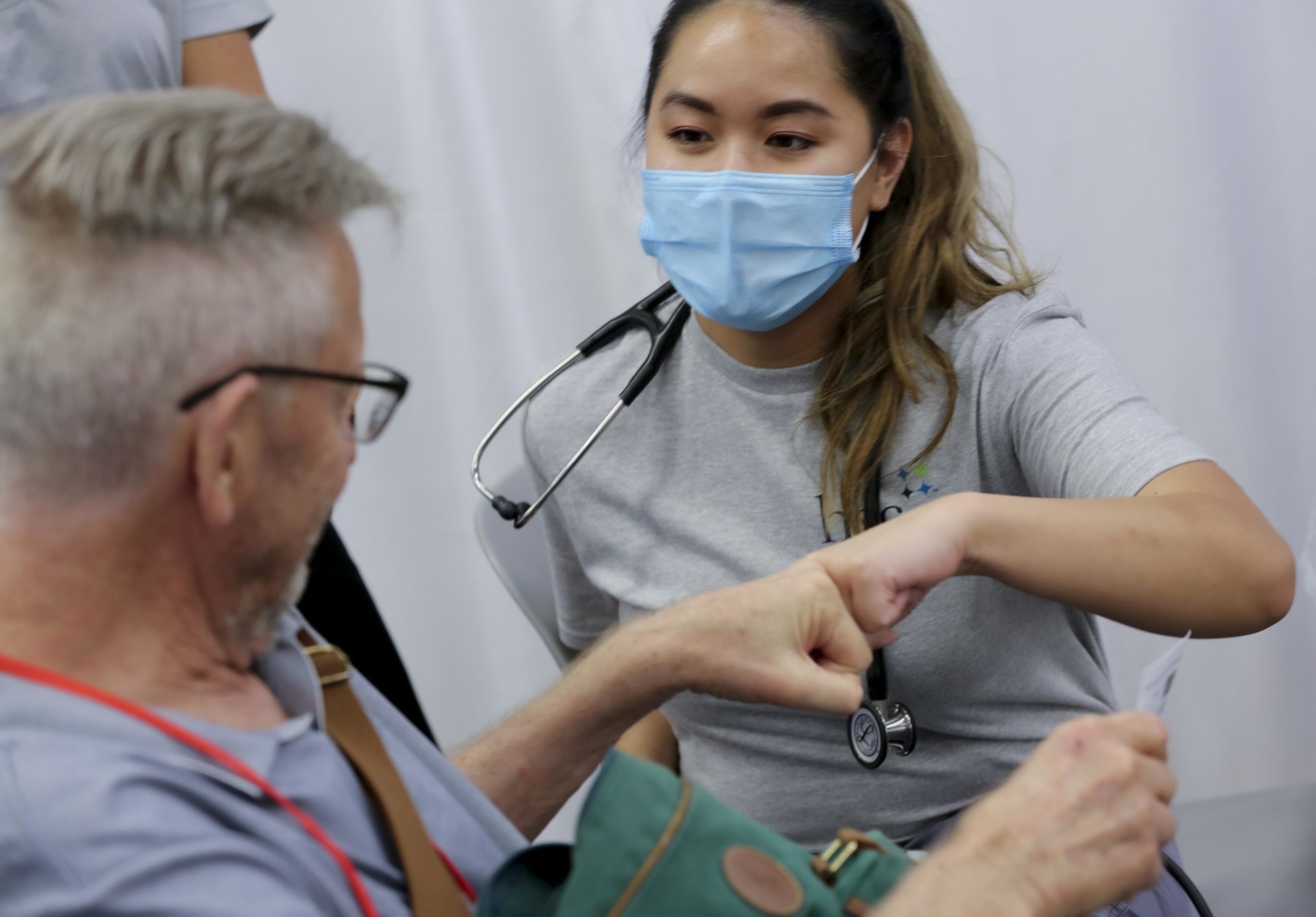
Community
Latest news

HSC names Dr. Christopher Ray as new Deputy Provost
The University of North Texas Health Science Center at Fort Worth has named Dr. Christopher Ray as the new deputy...

HSC launches One Pill Kills Campaign to combat fentanyl
A synthetic opioid that’s considered exponentially more addictive than heroin, fentanyl is now the leading cause of death for Americans...

Dr. Dimitrios Karamichos named HSC School of Biomedical Sciences interim...
Dimitrios Karamichos, PhD, has been appointed interim dean of The University of North Texas Health Science Center at Fort Worth...

Dr. Annesha White named College of Pharmacy Interim Dean
Annesha White, PharmD, MS, PhD, was named Interim Dean of HSC College of Pharmacy as of Sept. 8, and she...

Events




Social media